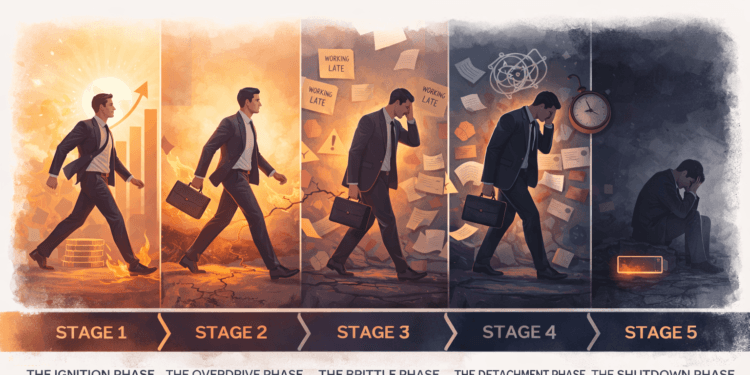
The Stages of Burnout in High Achievers
You can be a high performer and still be in trouble.
Not because you’re incapable. Because you’re adaptable.
High achievers are experts at compensating: more focus, more control, more hours, more systems, more “I’ll handle it.” That works, until your body quietly decides it can’t keep funding your life at the current rate.
And that’s why burnout in high achievers often shows up in stages. Subtle at first. “Normal stress” at first. Then a slow narrowing of your capacity, until you wake up one day and realize rest isn’t restoring you, motivation feels unreliable, and your nervous system seems permanently stuck in overdrive.
This article breaks down a practical five-stage pattern many high achievers move through, grounded in what we know about burnout symptoms, chronic stress effects, and nervous system dysregulation. It also gives you a stage-matched pathway for nervous system regulation, including vagus nerve breathing, parasympathetic nervous system activation, gut-brain support, and reality-based strategies that don’t require you to quit your life.
Why high achievers burn out in stages
Burnout isn’t a switch. It’s a progression.
You don’t go from “fine” to “broken.” You go from normal stress response → chronic stress adaptation → diminished recovery → nervous system instability → forced slowdown.
That progression is often hard to see from the outside because high achievers stay functional longer than most. They can produce through exhaustion. They can think through anxiety. They can keep it together socially while their body is quietly doing something else.
Two things make the “stages” pattern particularly common in high achievers:
First, burnout is defined as a response to chronic workplace stress that hasn’t been successfully managed, not a one-time event. [1]
Second, chronic stress doesn’t just affect mood. It affects multiple body systems—musculoskeletal, cardiovascular, endocrine, gastrointestinal and nervous systems—meaning the symptoms often appear across sleep, digestion, energy, focus, and emotional reactivity. [2]
So a stage model isn’t a claim that burnout unfolds the same way for everyone. It’s a way to make a complex pattern visible early—when you still have leverage.
Burnout is not just stress
There’s a reason “burnout” lands differently than “I’m stressed.”
In the World Health Organization[3] ICD‑11 framing, burnout is described as a syndrome resulting from chronic workplace stress that hasn’t been successfully managed, characterized by exhaustion, increased mental distance/cynicism, and reduced professional efficacy. It’s also explicitly framed as an occupational phenomenon rather than a medical condition. [4]
In the research tradition led by Christina Maslach[5], burnout is commonly discussed using the same three dimensions: exhaustion, cynicism/detachment, and reduced efficacy. [6]
Where people get stuck is assuming burnout is only “too much work.”
But occupational research has repeatedly shown burnout is strongly shaped by the demand–resource equation around you. The Job Demands–Resources model proposes that job demands are primarily related to exhaustion, while lack of job resources is primarily related to disengagement. [7]
That matters because a lot of high achievers keep trying to solve burnout with personal tools alone—more discipline, better morning routines, a new supplement stack—while returning daily to a system that keeps producing the same physiological outputs.
If you want how to recover from burnout, the strategy has to match the mechanism.
The burnout nervous system
If you’ve been searching phrases like:
- nervous system dysregulation
- overactive nervous system
- how to calm nervous system
- fight or flight symptoms
- symptoms of nervous system dysregulation
- how to reset nervous system
…you’re probably noticing something important:
Your body isn’t responding to rest the way it used to.
Chronic stress effects change your baseline
Chronic stress is not “in your head.” The American Psychological Association[8] summarizes stress as a whole-body phenomenon affecting multiple systems of the body, including the nervous system and gastrointestinal system. [9]
Mayo Clinic[10] similarly notes that long-term activation of the stress response system and prolonged exposure to stress hormones such as cortisol can disrupt many body processes and increase risk for problems like sleep disruption, digestive issues, muscle tension, weight gain, and memory/focus problems. [11]
That list overlaps almost perfectly with what people call chronic stress symptoms in real life: tight body, shallow breathing, poor sleep, irritable digestion, brain fog, low resilience.
Allostatic load explains why “a weekend off” doesn’t fix it
A key research framework here is allostatic load—the wear-and-tear that accumulates when stress-response systems are activated too often or don’t shut off efficiently. The classic model describes types of allostatic load including frequent activation and failure to shut off after stress. [12]
For high achievers, this is the missing explanation:
If your body has been running stress physiology daily for months or years, your “baseline” can shift. You can stop working and still feel activated because the system has learned activation as the default.
Nervous system dysregulation is often state rigidity
Your autonomic nervous system is designed to shift between activation and recovery. Cleveland Clinic[13] describes the autonomic nervous system as the network that controls automatic processes and highlights the balancing act between sympathetic activation and parasympathetic downshifting. [14]
When that system loses flexibility, you get what many people mean by nervous system dysregulation: difficulty transitioning out of survival-mode states.
That may show up as hyperarousal—senses and thoughts working overtime as if you’re in fight-or-flight with no present danger. Cleveland Clinic describes hyperarousal as a prolonged fight-or-flight response that’s activated too easily or stays active too long. [15]
It also shows up as sleep disruption. In insomnia science, the hyperarousal model is well-supported: hyperarousal across physiological and cognitive-emotional domains plays a key role in insomnia pathophysiology. [16]
So if your burnout includes 3 a.m. wake-ups, “tired but wired,” racing thoughts, and shallow sleep, you’re not simply failing at relaxation. You’re dealing with a nervous system that won’t downshift.
Fight, flight, freeze, and fawn in high achievers
Fight or flight symptoms are commonly described as increased heart rate and blood pressure, rapid breathing, increased sweating, a surge of energy/strength, slowed digestion, and dilated pupils. [17]
But high achievers often don’t notice fight/flight as “panic.” They experience it as:
- constant urgency
- inability to sit still
- productivity as self-soothing
- irritability and tightness
- digestive disruption under pressure
Freeze is different. In research, freezing responses are discussed through constructs like tonic immobility—an evolved defence response involving physical immobility under extreme threat. [18]
High achiever freeze often looks like “functional shutdown”: staring at the screen, procrastination that feels like paralysis, emotional numbness, a heavy body, “I can’t.”
Fawn is not an official medical category, but it’s a widely used trauma-informed term describing appeasement and people-pleasing as a threat-reduction strategy. [19]
In high-achieving workplaces, fawn can look like over-accommodating, over-agreeing, and chronic boundary violations while staying polite.
When you understand these patterns, the stages of burnout become easier to recognize—because you stop looking for a meltdown and start looking for nervous system drift.
The stages of burnout in high achievers
Before we map stages, one important clinical truth:
There is no universally accepted, medically standardized “five-stage burnout progression.” Burnout has multiple competing models and measurement debates, and researchers disagree about which dimension comes first (exhaustion first vs detachment first, for example). [20]
Stage models are best treated as practical maps, not rigid diagnostic ladders.
With that said, a staged pattern does show up repeatedly in high achievers, and it aligns with what we know about job stress, burnout dimensions, and stress physiology. [21]
Below is a five-stage pattern that integrates:
- the WHO/Maslach burnout dimensions (exhaustion, cynicism, reduced efficacy) [22]
- the job demands/resources mechanism [23]
- the stress physiology baseline shift (allostatic load) [12]
- the nervous system dysregulation pattern (hyperarousal, freeze) [24]
The ignition phase
This is the stage high achievers romanticize.
You care. You’re ambitious. You feel responsible. You’re “handling it.”
What it feels like
You’re busy, but competent. You feel pressure, but it’s paired with purpose. You may even feel a certain proud intensity—like stress proves you matter.
Early signs of burnout
You start borrowing from the basics:
- sleep becomes slightly shorter or more irregular
- meals become rushed or inconsistent
- exercise becomes either excessive or disappears
- you begin thinking about work during rest
You may notice mild fight or flight symptoms: tight chest, shallow breathing, jaw tension, faster heart rate in the evening. [25]
What’s happening underneath
Your body is doing exactly what it’s designed to do: mobilize energy to meet demand. The problem begins when there is insufficient recovery between mobilizations—when stress activation becomes frequent. That’s one major pathway into allostatic load. [12]
Real-life scenario
A senior manager takes on “just one more project.” They stay late, skip lunch, and tell themselves they’ll catch up on rest later. It works—until it doesn’t.
What to do in this phase
Don’t jump to dramatic changes. Do one thing: reduce activation frequency.
Your first “how to regulate nervous system” move is not a two-hour routine. It’s micro-regulation: short, repeatable downshifts that keep daily stress from becoming your baseline. [26]
The overdrive phase
This is where high achievers start to confuse adaptation with resilience.
You aren’t just busy anymore. You’re running a tightly managed system to keep performance stable.
What it feels like
You’re still productive, but you’re less available in your own life. Weekdays blur. Weekends feel like a recovery debt payment.
Signs of burnout (high-functioning version)
– rest feels unrefreshing
– irritability increases
– focus requires more effort
– you start leaning on stimulants or numbing behaviours
– you feel “wired” at night, even when you’re exhausted
This is classic overactive nervous system territory: mobilization without clean downshifts.
What’s happening underneath
Chronic activation can impair sleep and cognition, weakening recovery and increasing stress vulnerability. Mayo Clinic explicitly notes that chronic stress can contribute to sleep problems and memory/focus problems. [11]
You also begin losing psychological detachment—your brain keeps running work loops during off time, which blunts recovery. That’s part of why time off often helps temporarily and then fades quickly when work resumes. [27]
Real-life scenario
A physician finishes a demanding shift and can’t downshift at home. They scroll, snack, and respond to messages “just in case.” They’re “resting,” but their nervous system doesn’t register safety.
What to do in this phase
Start building parasympathetic nervous system activation into your day in small doses. The parasympathetic system is the network that helps your body relax after stress and supports functions like digestion when you feel safe. [28]
The brittle phase
This is where many high achievers first admit something is wrong—because performance becomes unpredictable.
What it feels like
You can still perform, but you feel brittle: one more demand feels like too much.
Common burnout symptoms here
– brain fog, forgetfulness, decision fatigue
– deeper sleep disruption (waking early, waking at night, restless sleep)
– emotional volatility (snapping, tearing up unexpectedly)
– increased somatic symptoms: headaches, gut issues, muscle pain
Chronic stress affects multiple body systems, which is why this phase often looks like “everything at once.” [2]
What’s happening underneath
Hyperarousal becomes more obvious. Insomnia science supports hyperarousal as a key mechanism—your system stays activated across day and night. [29]
You may also begin experiencing the gut stress loop more strongly. The fight-or-flight response slows digestion so the body can divert energy to the threat response. [30]
If you’ve been searching for stress and digestion or gut-brain axis anxiety, this is often the phase where people finally connect their anxiety with gut symptoms. Reviews describe the microbiota–gut–brain axis as a bidirectional communication pathway involved in anxiety mechanisms through neural, endocrine, and immune pathways. [31]
Real-life scenario
A tech leader wakes up at 3 a.m., their mind racing. They compensate with more caffeine, which helps in the morning but worsens at night. They start to feel “tired but wired” and can’t relax even on weekends.
What to do in this phase
You need active nervous system training, not more passive rest.
One of the most evidence-supported tools here is vagus nerve breathing (slow, voluntary breathing). A systematic review and meta-analysis found voluntary slow breathing increases vagally mediated heart rate variability, supporting its role in influencing parasympathetic-linked regulation. [32]
In simple terms: longer exhales and slower breathing rhythms can help take your system out of emergency mode.
The detachment phase
This phase often scares high achievers because it looks like personality change.
You stop caring the way you used to.
What it feels like
You feel numb, cynical, or emotionally distant. You do your job, but meaning is thin. You might fantasize about quitting. You might feel guilty for feeling this way.
In the WHO’s burnout definition, increased mental distance/negativism/cynicism is a core dimension. [1]
How freeze and fawn show up here
– Freeze symptoms in high achievers: avoidance, paralysis, procrastination, dissociation-like numbness, “I can’t start.” Tonic immobility research describes freeze-like immobility responses under extreme stress and threat contexts. [18]
– Fawn symptoms in high achievers: appeasing leadership, people-pleasing, over-agreeing, chronic boundary erosion, “I can’t say no.” The fawn response is commonly described as a please-and-appease pattern linked to threat avoidance in relational contexts. [19]
This phase is where many people become “nice” and resentful—compliant on the outside, depleted on the inside.
What’s happening underneath
Detachment can function like a conserving strategy: if you can’t reduce demands, the system reduces emotional investment to survive. Burnout theory debates the sequence of dimensions (detachment first vs exhaustion first), but detachment is consistently recognized as part of the syndrome. [33]
Real-life scenario
A high-achieving educator becomes “checked out.” They still teach, still grade, still perform, but feel emotionally disconnected and irritated by students and colleagues. Their body is exhausted, and their nervous system is overreactive.
What to do in this phase
The primary intervention is not “think more positively.” It’s restoration of capacity and boundaries—because your nervous system is signalling a resource crisis.
The Job Demands–Resources framework is blunt: high demands push exhaustion; low resources push disengagement. [23]
Detachment often decreases when resources increase: control, clarity, support, staffing, and realistic workload.
The shutdown phase
This is the phase people call “crashing.”
Your body enforces a stop.
What it feels like
– exhaustion that sleep doesn’t fix
– frequent illness, or slow recovery
– severe brain fog
– anxiety spikes or emotional collapse
– you can’t access motivation reliably
– you may start to feel unsafe in your own body
This phase can be accompanied by more intense somatic symptoms because chronic stress disrupts multiple processes, including immune and cardiovascular systems, sleep and cognition. [34]
A clinical note
Burnout can overlap with depression and anxiety, and if you’re experiencing persistent low mood, hopelessness, panic, or severe impairment, you deserve assessment and support. Burnout itself is not classified as a medical condition by WHO, but it is a valid reason to seek care. [35]
Real-life scenario
A legal partner takes a vacation, feels slightly better, and then relapses within weeks of returning. This rebound is consistent with research showing vacation relief can fade out after resuming work, with burnout returning toward pre-vacation levels by weeks post-vacation. [27]
What to do in this phase
Stage five requires a structured rebuild: sleep stabilisation, nervous system regulation training, workload renegotiation, and systematic reduction of allostatic load drivers. [36]
This is where “just rest” fails—because rest reduces demand temporarily but doesn’t retrain the baseline.
How to recover from burnout
If you want how to recover from burnout, the most useful approach is stage-matched. What works in stage one may be insufficient in stage four.
Below is a practical recovery protocol you can actually implement in a high-demand life, built around nervous system healing, not perfect wellness routines.
Stabilize your baseline first
Your first job is to stop volatility.
In burnout, instability is the enemy: irregular sleep, irregular meals, constant stimulation, constant availability.
Stabilization is a nervous system intervention because your autonomic system thrives on predictable safety cues. [26]
Start with two anchors:
A consistent wake time most days (even if bedtime shifts).
A daily shutdown ritual that tells your brain work is over (same time, same sequence).
Train nervous system regulation with non-negotiable micro-practice
If you’re searching for how to regulate nervous system, the answer is not one hack. It’s repeated practice.
The most evidence-backed “vagus nerve exercise” is slow breathing.
Vagus nerve breathing protocol
– inhale gently for about four seconds
– exhale for about six seconds
– repeat for five minutes
Voluntary slow breathing has been shown in meta-analytic work to increase vagally mediated HRV, supporting its role in parasympathetic-linked regulation. [37]
This is natural ways to calm anxiety in its most physiologically honest form: you’re not forcing calm; you’re changing state.
Make parasympathetic activation visible in your day
Most high achievers only try to relax at night. That’s too late.
Build “micro-downshifts” into the workday:
After intense meetings: three minutes of slow breathing.
Between tasks: one minute of shoulder drop + long exhale.
After work: ten-minute decompression walk, no phone.
This is nervous system regulation as a system, not an event.
Repair sleep like a clinical priority
If you’re in the brittle/detachment/shutdown stages, sleep must become non-negotiable—not through sleep hygiene perfection, but through evidence-based treatment when needed.
The American College of Physicians[38] recommends cognitive behavioural therapy for insomnia (CBT‑I) as the initial treatment for chronic insomnia disorder in adults. [39]
If you’re waking at 2–4 a.m. with racing thoughts or lying awake for long periods, CBT‑I principles (stimulus control, sleep consolidation) can be more effective than adding more bedtime rituals. [40]
Stabilize the gut-brain axis instead of treating digestion as “separate.”
High achievers often treat digestion as an inconvenience. That’s a mistake.
Stress inhibits digestion. When fight-or-flight activates, digestion can slow or stop as energy is diverted to the perceived threat response. [30]
If you’re dealing with stress and digestion symptoms—bloating, urgency, reflux, nausea during pressure—supporting digestion is nervous system work.
For gut-brain axis anxiety, the science is increasingly clear that gut–brain, immune, endocrine, and neural pathways interact in anxiety mechanisms. [31]
Practical, non-extreme support looks like:
Regular meal timing (predictability reduces physiological stress).
Slower eating (sympathetic eating patterns worsen gut sensitivity).
A simple “post-meal downshift” (five minutes sitting, long exhales).
If symptoms are persistent or severe, clinical evaluation.
Adaptogens for stress
Many readers want adaptogens for stress. Some have evidence, but the category is not risk-free.
Ashwagandha is among the most studied, and clinical trials and systematic reviews suggest it may reduce stress and anxiety in some populations. [41]
But safety matters. The National Center for Complementary and Integrative Health[42] notes that short-term use may be safe for some people, but adverse effects occur; rare liver injury cases have been reported, and it should be avoided in pregnancy and breastfeeding. [43]
If you choose to use adaptogens as part of holistic stress management:
Use them as support, not as the foundation.
Choose reputable products.
Avoid mixing multiple new supplements at once.
Talk to a clinician if you have liver issues, thyroid conditions, pregnancy/breastfeeding, or medications.
Change the demand–resource equation
This is the step high achievers resist—because it feels like losing.
It’s actually how you recover.
The job demands–resources model was built to explain burnout for a reason: demands drive exhaustion; lack of resources drives disengagement. [44]
Choose one demand to reduce in the next month and one resource to increase:
Reduce: one meeting, one after-hours expectation, one project.
Increase: control over schedule, admin support, clearer priority rules, and protected focus blocks.
This is what stops relapse. A vacation can reduce symptoms temporarily, but research shows the relief can fade after returning to work if the system doesn’t change. [27]
Common mistakes high achievers make
High achievers don’t stay burned out because they don’t try. They stay burned out because they apply stress tactics to a burnout problem.
Mistake: treating burnout symptoms like a motivation issue
Burnout involves exhaustion, cynicism/distance, and reduced efficacy. More effort doesn’t resolve that triad; it often intensifies it. [22]
Mistake: using rest as compensation rather than redesign
Time off helps, then fades when you re-enter the same workload. Vacation relief and fade-out research highlight how burnout can rebound after work resumption. [27]
Mistake: trying to calm your nervous system only at night
If the day trains hyperarousal, nighttime can’t undo it fully. Hyperarousal models show that insomnia involves sustained arousal across systems, not only bedtime habits. [29]
Mistake: mistaking fawn for professionalism
If your nervous system uses appeasement to avoid conflict, you’ll keep violating your boundaries in the name of being “easy to work with.” Fawn patterns are described as please-and-appease strategies linked to threat reduction in relational contexts. [19]
Mistake: relying on supplements while keeping the same inputs
Adaptogens can support, but no supplement reverses chronic workplace stress and allostatic load on its own. [45]
A deeper rebuild
If you recognized yourself in the later stages—brittleness, detachment, shutdown—then the next move is usually not another tip.
It’s a structured system.
On the OOverall Health[46] program page, The Calm Rebuild™ is described as a 12‑week live clinical experience and a four-phase “nervous system calibration journey” designed for high-capacity professionals who are done managing burnout and want to resolve it at the root. [47]
The page describes phases focused on nervous system calibration (including vagus nerve activation and gut-brain stabilization), identity shift (perfectionism and overthinking patterns), cognitive capacity expansion, and long-term resilience systems. [47]
If you’re dealing with a burnout progression, that staged structure matters—because burnout recovery is not one intervention. It’s rebuilding baseline safety in the body and building “self-correcting” nervous system skills that hold when stress returns. [48]
Program link (as provided):
Conclusion
High achievers don’t burn out because they’re fragile. They burn out because they’re trained to perform through stress signals—and the nervous system keeps score.
Burnout, in the WHO framing, is chronic workplace stress that hasn’t been successfully managed, marked by exhaustion, cynicism/mental distance, and reduced efficacy. [1]
Chronic stress affects the body across multiple systems, which is why burnout symptoms often show up as sleep disruption, digestion issues, muscle tension, brain fog, and emotional volatility—not just “feeling tired.” [2]
Allostatic load explains why the body can stay activated even when you stop working: repeated activation and failure to shut off after stress creates cumulative strain. [12]
The way out is not forcing calm.
It’s nervous system regulation done consistently: micro-downshifts, vagus nerve breathing, sleep repair when insomnia is present, gut-brain support, and real changes to the demand–resource equation that created the burnout nervous system in the first place. [49]
[1] [4] [22] [35] [38] [46] Burn-out an occupational phenomenon
[2] [8] [9] [10] Stress effects on the body
https://www.apa.org/topics/stress/body?utm_source=chatgpt.com
[3] [12] [36] [45] Stress, adaptation, and disease. Allostasis and allostatic load
https://pubmed.ncbi.nlm.nih.gov/9629234/?utm_source=chatgpt.com
[5] [13] [30] Stress and The Sensitive Gut
[6] Understanding the burnout experience: recent research … – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC4911781/?utm_source=chatgpt.com
[7] [21] [23] [44] The job demands-resources model of burnout
https://pubmed.ncbi.nlm.nih.gov/11419809/?utm_source=chatgpt.com
[11] [34] Chronic stress puts your health at risk
[14] [26] Autonomic Nervous System: What It Is, Function & Disorders
https://my.clevelandclinic.org/health/body/23273-autonomic-nervous-system?utm_source=chatgpt.com
[15] [24] Hyperarousal: What It Is, Causes, Symptoms & Treatment
https://my.clevelandclinic.org/health/symptoms/hyperarousal?utm_source=chatgpt.com
[16] [29] [42] The hyperarousal model of insomnia: a review …
https://pubmed.ncbi.nlm.nih.gov/19481481/?utm_source=chatgpt.com
[17] [25] Stress response (fight-or-flight response)
[18] Tonic immobility differentiates stress responses in PTSD – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC5102644/?utm_source=chatgpt.com
[19] Fawn Response: Adding to The Fight, Flight, or Freeze …
https://psychcentral.com/health/fawn-response?utm_source=chatgpt.com
[20] [33] Burnout: A Review of Theory and Measurement – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC8834764/?utm_source=chatgpt.com
[27] Effects of a Respite From Work on Burnout: Vacation Relief …
[28] Parasympathetic Nervous System (PSNS): What It Is & …
[31] Mechanisms of microbiota-gut-brain axis communication in …
[32] [37] [49] Effects of voluntary slow breathing on heart rate and …
https://pubmed.ncbi.nlm.nih.gov/35623448/?utm_source=chatgpt.com
[39] [40] Management of Chronic Insomnia Disorder in Adults
https://pubmed.ncbi.nlm.nih.gov/27136449/?utm_source=chatgpt.com
[41] Ashwagandha: Is it helpful for stress, anxiety, or sleep?
https://ods.od.nih.gov/factsheets/Ashwagandha-HealthProfessional/?utm_source=chatgpt.com
[43] Ashwagandha: Usefulness and Safety – nccih
https://www.nccih.nih.gov/health/ashwagandha?utm_source=chatgpt.com